Abstract
INTRODUCTION
U.S. Hispanic women suffer a disproportionate burden of cervical cancer, with incidence and mortality rates almost twice that of whites. Community health workers, or promotoras, are considered a potential strategy for eliminating such racial and ethnic health disparities. The current study is a randomized trial of a promotora-led educational intervention focused on cervical cancer in a local Hispanic community.
METHODS
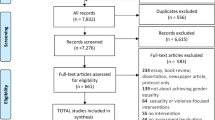
Four promotoras led a series of two workshops with community members covering content related to cervical cancer. Sociodemographic characteristics, cervical cancer risk, previous screening history, cervical cancer knowledge, and self-efficacy were measured by a pre-intervention questionnaire. The post-intervention questionnaire measured the following outcomes: cervical cancer knowledge (on a 0–6 scale), self-efficacy (on a 0–5 scale), and receipt of Pap smear screening during the previous 6 months (dichotomous). Univariate analyses were performed using chi square, t-test, and the Mann–Whitney test. Multivariate logistic regression was used to model the association between explanatory variables and receipt of Pap smear screening.
RESULTS
There were no statistically significant differences between the two experimental groups at baseline. Follow-up data revealed significant improvements in all outcome measures: Pap smear screening (65% vs. 36%, p-value 0.02), cervical cancer knowledge (5.4 vs. 3.5, p-value < 0.001), and self-efficacy (4.7 vs. 4.0, p-value 0.002). In multivariate analysis, cervical cancer knowledge (OR 1.68, 95% CI 1.10-2.81) and intervention group assignment (OR 6.74, 95% CI 1.77-25.66) were associated with receiving a Pap smear during the follow-up period.
DISCUSSION
Our randomized trial of a promotora-led educational intervention demonstrated improved Pap screening rates, in addition to increased knowledge about cervical cancer and self-efficacy. The observed association between cervical cancer knowledge and Pap smear receipt underscores the importance of educating vulnerable populations about the diseases that disproportionately affect them. Future research should evaluate such programs on a larger scale, and identify novel targets for intervention.

Similar content being viewed by others
References
Guzman B. Census 2000 brief: The Hispanic population. Washington, DC: U.S. Department of Commerce, Economics and Statistics Administration, U.S. Census; 2001.
U.S. Census Bureau. U.S. Interim Projections by Age, Sex, Race, and Hispanic Origin: 2000-2050. Available from: http://www.census.gov/population/www/projections/usinterimproj/. Accessed June 11, 2010
National healthcare disparities report. Washington, DC: U.S. Department of Health and Human Services, Agency for Healthcare Research and Quality; 2008.
Smedley B, Stith A, Nelson A, eds. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The Institute of Medicine: The National Academies Press; 2003.
Schlotthauer A, Badler A, Cook S, Perez D, Chin M. Evaluating interventions to reduce health care disparities: An RWJF program. Health Aff. 2008;27(2):568–73.
Howe H, Wu X, Ries L, Cokkinides V, Ahmed F, Jemal A, et al. Annual report to the nation on the status of cancer, 1975-2003, featuring cancer among U.S. Hispanic/Latino populations. Cancer. 2006;107(8):1711–42.
Cancer facts and figures for Hispanics/Latinos 2009-2011. Atlanta, GA: American Cancer Society; 2009.
Barnholtz-Sloan J, Petel N, Rollison D, Kortepeter K, MacKinnon J, Giuliano A. Incidence trends of invasive cervical cancer in the United States by combined race and ethnicity. Canc Causes Contr. 2009;20:1129–38.
Cancer prevention and early detection facts and figures 2009. Atlanta, GA: American Cancer Society; 2009.
Bazargan M, Bazargan S, Farooq M, Baker R. Correlates of cervical cancer screening among underserved Hispanic and African-American women. Prev Med. 2004;39:465–73.
Holschneider C, Felix J, Satmary W, Johnson M, Sandweiss L, Montz F. A single-visit cervical carcinoma prevention program offered at an inner city church. Cancer. 1999;86(12):2659–67.
Sirovich B, Welch H. The frequency of Pap smear screening in the United States. J Gen Intern Med. 2004;19(3):243–50.
Arredondo E, Pollak K, Costanzo P. Evaluating a stage model in predicting monolingual Spanish-speaking Latinas' cervical cancer screening practices: The role of psychosocial and cultural predictors. Health Educ Behav. 2008;35(6):791–805.
Johnson C, Mues K, Mayne S, Kiblawi A. Cervical cancer screening among immigrants and ethnic minorities: A systematic review using the health belief model. J Low Genit Tract Dis. 2008;12(3):232–41.
Austin L, Ahmad F, McNally M, Stewart D. Breast and cervical cancer screening in Hispanic women: A literature review using the health belief model. Womens Health Issues. 2002;12(3):122–8.
Ackerson K, Gretebeck K. Factors influencing cancer screening practices of underserved women. J Am Acad Nurse Pract. 2007;19:591–601.
Garbers S, Chiasson M. Inadequate functional health literacy in Spanish as a barrier to cervical cancer screening among immigrant Latinas in New York City. Prev Chron Dis. 2004;1(4):1–10.
Rodriguez M, Ward L, Perez-Stable E. Breast and cervical cancer screening: Impact of health insurance status, ethnicity, and nativity of Latinas. Ann Fam Med. 2005;3:235–41.
Byrd T, Chavez R, Wilson K. Barriers and facilitators of cervical cancer screening among Hispanic women. Ethn Dis. 2007;17(1):129–34.
Cadarelli R, Kurian A, Pandya V. Having a personal healthcare provider and recepit of adequate breast and cervical cancer screening. J Am Board Fam Med. 2010;23(1):75–81.
Mead H, Cartwright-Smith L, Jones K, Ramos C, Siegel B, Woods K. Racial and ethnic disparities in U.S. health care: a chartbook. New York: The Commonwealth Fund; 2008.
Flores K, Bencomo C. Preventing cervical cancer in the Latina population. J Womens Health. 2009;18(12):1935–43.
Goel M, Wee C, McCarthy E, Davis R, Ngo-Metzger Q, Phillips R. Racial and ethnic disparities in cancer screening: The importance of foreign birth as a barrier to care. J Gen Intern Med. 2003;18(12):1028–35.
Witmer A, Seifer S, Finocchio L, Leslie J, O'Neil E. Community health workers: integral members of the health care workforce. Am J Public Health. 1995;85:1055–8.
Perez L, Martinez J. Community health workers: Social justice and policy advocates for community health and well-being. Am J Public Health. 2008;98:11–4.
Love M, Gardner K, Legion V. Community health workers: What they are and what they do. Health Educ Behav. 1997;24(4):510–22.
Humphrey J, Jameson L, Beckham S. Overcoming social and cultural barriers to care for patients with diabetes. West J Med. 1997;167:138–44.
Ingram M, Torres E, Redondo F, Bradford G, Wang C, O'Toole M. The impact of promotoras on social support and glycemic control among members of a farmworker community on the U.S.-Mexico border. Diab Educ. 2007;33(Suppl 6):172S–8.
Lujan J, Ostwald S, Ortiz M. Promotora diabetes intervention for Mexican Americans. Diab Educ. 2007;33(4):660–70.
Thompson J, Horton C, Flores C. Advancing diabetes self-management in the Mexican-American population: A community health worker model in a primary care setting. Diab Educ. 2007;33:159S–65.
Campbell M, James A, Farrell M, Tessaro I. Improving multiple behaviors for colorectal cancer prevention among African American church members. Health Psychol. 2004;23(5):492–502.
Erwin D, Spatz T, Stotts R, Hollenberg J. Increasing mammography practice by African American women. Cancer Pract. 1999;7(2):78–85.
Koval A, Riganti A, Foley K. CAPRELA (Cancer Prevention for Latinas): Findings of a pilot study in Winston-Salem, Forsyth County. NC Med J. 2006;67(1):9–15.
Paskett E, Tatum C, Rushing J, Michielutte R, Bell R, Foley K, et al. Randomized trial of an intervention to improve mammography utilization among a triracial rural population of women. J Natl Cancer Inst. 2006;98:1226–37.
Welsh A, Sauaia A, Jocobellis J, Min S, Byers T. The effect of two church-based interventions on breast cancer screening rates among Medicaid-insured Latinas. Prev Chron Dis. 2005;2(4):1–11.
Balcazar H, Alvarado M, Cantu F, Pedregon V, Fulwood R. A promotora de salud model for addressing cardiovascular disease risk factors in the U.S.-Mexico border region. Prev Chron Dis. 2009;6(1):1–8.
Hill M, Han H, Dennison C, Kim M, Roary M, Blumenthal R, et al. Hypertension care and control in underserved African American men: Behavioral and physiologic outcomes at 36 months. Am J Hypertens. 2003;16:906–13.
Krieger J, Collier C, Song L, Martin D. Linking community-based blood pressure measurement to clinical care: A randomized controlled trial of outreach and tracking by community health workers. Am J Public Health. 1999;89:856–61.
Staten L, Gregory-Mercado K, Ranger-Moore J, Will J, Giuliano A, Ford E, et al. Provider counseling, health education, and community health workers: The Arizona WISEWOMEN project. J Womens Health. 2004;13(5):547–56.
Fox P, Porter P, Lob S, Boer J, Rocha D, Adelson J. Improving asthma-related health outcomes among low-income, multiethnic, school-aged children: Results of a demonstration project that combined continuous quality improvement and community health worker strategies. Pediatrics. 2007;120:e902–11.
Krieger J, Takaro T, Song L, Weaver M. The Seattle-King County healthy homes project: A randomized, controlled trial of a community health worker intervention to decrease exposure to indoor asthma triggers. Am J Public Health. 2005;95:652–9.
Martin M, Hernandez O, Naureckas E, Lantos J. Reducing home triggers for asthma: The Latino community health worker approach. J Asthma. 2006;43(5):369–74.
Parker E, Israel B, Robbins T, Mentz G, Lewis T. Evaluation of Community Action Against Asthma: A community health worker intervention to improve children's asthma-related health by reducing household environmental triggers for asthma. Health Educ Behav. 2008;35(3):376–95.
Thyne S, Marmor A, Madden N, Herrick G. Comprehensive asthma management for underserved children. Paediatr Perinat Epidemiol. 2007;21(Suppl 3):29–34.
Hunter J, De Zapien J, Papenfuss M, Fernandez M, Meister J, Giuliano A. The impact of a promotora on increasing routine chronic disease prevention among women aged 40 and over at the U.S.-Mexico border. Health Educ Behav. 2004;31(4):18S–28.
Navaie-Waliser M, Martin S, Tessaro I, Campbell M, Cross A. Social support and psychological functioning among high-risk mothers: The impact of the Baby Love Maternal Outreach Program. Public Health Nurs. 2000;17(4):280–91.
Rogers M, Peoples-Sheps M, Suchindran C. Impact of a social support program on teenage prenatal care use and pregnancy outcomes. J Adolesc Health. 1996;19:132–40.
Watkins E, Larson K, Harlan C, Young S. A model program for providing health services for migrant farmworker mothers and children. Public Health Rep. 1990;105(6):567–75.
O'Brien M, Squires A, Bixby R, Larson S. Role Development of Community Health Workers: An examination of selection and training processes in the intervention literature. Am J Prev Med. 2009;37(6S1):S262–9.
Martinez-Donate A. Using lay health advisors to promote breast and cervical cancer screening among Latinas: A brief qualitative review. Wis Med J. 2009;108(5):49–51.
Rhodes S, Foley K, Zometa C, Bloom F. Lay health advisor interventions among Hispanics/Latinos: A qualitative systematic review. Am J Prev Med. 2007;33(5):418–27.
Swider S. Outcome effectiveness of community health workers: An integrative literature review. Public Health Nurs. 2002;19(1):11–20.
Lewin S, Dick J, Pond P, Zwarenstein M, Aja G, van Wyk B, et al. Lay health workers in primary and community health care. Cochrane Database of Systematic Reviews 2005(1):1-104.
Community health worker national workforce study. Washington, DC: U.S. Department of Health and Human Services, Health Services and Resource Administration; 2007.
NIH. Cervical cancer consensus statement. 1996;14(1):1-38.
Margolis K, Lurie N, McGovern P, Tyrrell M, Slater J. Increasing breast and cervical cancer screening in low-income women. J Gen Intern Med. 1998;13:515–21.
Bird J, McPhee S, Ha N, Le B, Davis T, Jenkins C. Opening pathways to cancer screening for Vietnamese-American women: Lay health workers hold a key. Prev Med. 1998;27:821–9.
Fernandez M, Gonzales A, Tortolero-Luna G, Williams J, Saavedra-Embesi M, Chan W, et al. Effectiveness of Cultivando la Salud: A breast and cervical cancer screening promotion program for low-income Hispanic women. Am J Public Health. 2009;99:936–43.
Jandorf L, Bursac Z, Pulley L, Trevino M, Castillo A, Erwin D. Breast and cervical cancer screening among Latinas attending culturally specific educational programs. Progress in Community Health Partnerships. 2008;2(3):195–204.
Lam T, McPhee S, Mock J, Wong C, Doan H, Nguyen T, et al. Encouraging Vietnamese-American women to obtain Pap tests through lay health worker outreach and media education. J Gen Intern Med. 2003;18:516–24.
Navarro A, Senn K, McNicholas L, Kaplan R, Roppe B, Campo M. Por la Vida model intervention enhances use of cancer screening tests among Latinas. Am J Prev Med. 1998;15(1):32–41.
Navarro A, McNicholas L, Cruz M, McKennett M, Sanchez O, Senn K, et al. Development and implementation of a curriculum on cancer screening for small groups of Latino women. J Cancer Educ. 2007;22:186–90.
Navarro A, Senn K, Kaplan R, McNicholas L, Campo M, Roppe B. Por la Vida intervention model for cancer prevention in Latinas. J Natl Cancer Inst Monogr. 1995;18:137–45.
Theory at a glance: A guide for health promotion practice (2nd edition). Washington, DC: U.S. Department of Health and Human Services, National Institutes of Health; 2005.
Israel B, Eng E, Schultz A, Parker E, eds. Methods in community-based participatory research for health. San Francisco: John Wiley & Sons; 2005.
Squires A, O'Brien M. Becoming a promotora: a transformative process for female community health workers. under review Jan 2010
Hogenmiller J, Atwood J, Lindsey A, Johnson D, Hertzog M, Scott J. Self-efficacy scale for Pap smear screening participation in sheltered women. Nurs Res. 2007;56(6):369–77.
Marin G, Sobogal F, Marin B, Otero-Sabogal R, Perez-Stable E. Development of a short acculturation scale for Hispanics. Hisp J Behav Sci. 1987;9(2):183–205.
Martin M. Community health advisors effectively promote cancer screening. Ethn Dis. 2005;15(suppl 2):S214–6.
Berman PG. DR, Burger S. Community-based health workers: head start or false start towards health for all? Soc Sci Med. 1987;25(5):443–59.
Bullock K, McGraw S. A community capacity-enhancement approach to breast and cervical cancer screening among older women of color. Health Soc Work. 2006;31(1):16–25.
Hansen L, Feigl P, Modiano M, Lopez J, Sluder S, Moinpour C, et al. An educational program to increase cervical and breast cancer screening in Hispanic women. Cancer Nurs. 2005;28(1):47–53.
Larkey L. Las Mujeres Saludables: Reaching Latinas for breast, cervical, and colorectal cancer prevention and screening. J Community Health. 2006;31(1):69–77.
Park K, Park J, Park J, Kim H, Park B. Does health status influence intention regarding screening mammography? Japanese Journal of Clinical Oncology;Jan 2010 [ePub ahead of print]
Glanz K, Rimer B, Viswanath K, eds. Health behavior and health education: theory, research, and practice. 4th ed. San Francisco: John Wiley & Sons; 2008.
Ackerson K, Pohl J, Low L. Personal influencing factors associated with Pap smear testing and cervical cancer. Policy Polit Nurs Pract. 2008;9(1):50–60.
Anya S, Oshi D, Nwosu S. Knowledge, attitudes, and practice of female health professionals regarding cervical cancer and Pap smear. Niger J Med. 2005;14(3):283–6.
Kim K, Yu E, Chen E, Kim J, Kaufman M, Purkiss J. Cervical cancer screening knowledge and practices among Korean-American women. Cancer Nurs. 1999;22(4):297–302.
Mutyaba T, Mmiro F, Weiderpass E. Knowledge, attitudes, and practices on cervical cancer screening among the medical workers of Mulango Hospital, Uganda. BMC Med Educ. 2006;6:13–9.
Nelson W, Moser R, Gaffey A, Waldron W. Adherence to cervical cancer screening guidelines for U.S. women aged 25-64: Data from the 2005 Health Information National Trends Survey. J Womens Health. 2009;18(11):1759–68.
Sait K. Attitudes, knowledge, and practices in relation to cervical cancer and its screening among women in Saudi Arabia. Saudi Med J. 2009;30(9):1208–12.
Uysal A, Birsel A. Knowledge about cervical cancer risk factors and Pap testing behavior among Turkish women. Asian Pac J Cancer Prev. 2009;10(3):345–50.
Abraido-Lanza A, Chao M, Gates C. Acculturation and cancer screening among Latinas: Results from the National Health Interview Survey. Ann Behav Med. 2005;29(1):22–8.
Fernandez-Esquer M, Espinoza P, Ramirez A, McAlister A. Repeated Pap smear screening among Mexican-American women. Health Educ Res. 2003;18(4):477–87.
McDonald J, Kennedy S. Cervical cancer screening by immigrant and minority women in Canada. J Immigr Minor Health. 2007;9:323–34.
Watts L, Joseph N, Velasquez A, Gonzalez M, Munro E, Muzikansky A, et al. Understanding barriers to cervical cancer screening among Hispanic women. Am J Obstet Gynecol. 2009;201:199.e1–8.
Echeverria S, Carrasquillo O. The roles of citizenship status, acculturation, and health insurance in breast and cervical cancer screening among immigrant women. Med Care. 2006;44:788–92.
Gorin SH. JE. Cancer screening among Latino subgroups in the United States. Prev Med. 2005;40:515–26.
Shah M, Zhu K, Wu H, Potter J. Hispanic acculturation and utilization of cervical cancer screening in the US. Prev Med. 2006;42:146–9.
Acknowledgments
The authors thank the promotoras whose work is the subject of this article, and whose dedication to this study has been essential to its success. Their names are Susana Pimentel, Irma Zamora, Bertha Gonzalez, and Guadalupe Canchola. The authors would like to thank Giselle Dutcher and Darryl Powell for their help in the implementation of this study. We also thank Dr. Steven Larson for helping conceptualize and develop our community health worker program. We acknowledge our community partners involved in the design and ongoing implementation of the study: Puentes de Salud Health Center, the Mexican Consulate of Philadelphia, the Catholic Archdiocese of Philadelphia, and Juntos Mexicanos. The current study was supported by Grant Number UL1RR024134 from the National Center for Research Resources. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center for Research Resources or the National Institutes of Health. This paper was presented at the SGIM 33rd Annual Meeting in April 2010.
Conflict of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 366 kb)
Rights and permissions
About this article
Cite this article
O’Brien, M.J., Halbert, C.H., Bixby, R. et al. Community Health Worker Intervention to Decrease Cervical Cancer Disparities in Hispanic Women. J GEN INTERN MED 25, 1186–1192 (2010). https://doi.org/10.1007/s11606-010-1434-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-010-1434-6