ABSTRACT
BACKGROUND
Patients at risk for generating high health care expenditures often receive fragmented, low-quality, inefficient health care. Guided Care is designed to provide proactive, coordinated, comprehensive care for such patients.
OBJECTIVE
We hypothesized that Guided Care, compared to usual care, produces better functional health and quality of care, while reducing the use of expensive health services.
DESIGN
32-month, single-blind, matched-pair, cluster-randomized controlled trial of Guided Care, conducted in eight community-based primary care practices.
PATIENTS
The “Hierarchical Condition Category” (HCC) predictive model was used to identify high-risk older patients who were insured by fee-for-service Medicare, a Medicare Advantage plan or Tricare. Patients with HCC scores in the highest quartile (at risk for generating high health care expenditures during the coming year) were eligible to participate.
INTERVENTION
A registered nurse collaborated with two to five primary care physicians in providing eight services to participants: comprehensive assessment, evidence-based care planning, proactive monitoring, care coordination, transitional care, coaching for self-management, caregiver support, and access to community-based services.
MAIN MEASURES
Functional health was measured using the Short Form–36. Quality of care and health services utilization were measured using the Patient Assessment of Chronic Illness Care and health insurance claims, respectively.
KEY RESULTS
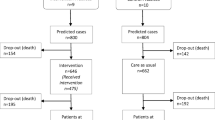
Of the eligible patients, 904 (37.8 %) gave written consent to participate; of these, 477 (52.8 %) completed the final interview, and 848 (93.8 %) provided complete claims data. In intention-to-treat analyses, Guided Care did not significantly improve participants’ functional health, but it was associated with significantly higher participant ratings of the quality of care (difference = 0.27, 95 % CI = 0.08–0.45) and 29 % lower use of home care (95 % CI = 3–48 %).
CONCLUSIONS
Guided Care improves high-risk older patients’ ratings of the quality of their care, and it reduces their use of home care, but it does not appear to improve their functional health.

Similar content being viewed by others
REFERENCES
Paez KA, Zhao L, Hwang W. Rising out-of-pocket spending for chronic conditions: a ten-year trend. Health Aff (Millwood). 2009;28(1):15–25.
Davis K, Schoen C, Stremikis K. Mirror, Mirror on the Wall: How the Performance on the U. S. Health Care System Compares Internationally. New York, New York: The Commonwealth Fund; 2010. http://www.commonwealthfund.org/~/media/Files/Publications/Fund%20Report/2010/Jun/1400_Davis_Mirror_Mirror_on_the_wall_2010.pdf. Accessed October 5, 2012.
Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press; 2001.
Anderson GF Chronic conditions: making the case for ongoing care. Partnership for Solutions; 2004. http://www.partnershipforsolutions.org/DMS/files/chronicbook2004.pdf. Accessed October 5, 2012.
Darer JD, Hwang W, Pham HH, Bass EB, Anderson G. More training needed in chronic care: a survey of U.S. physicians. Acad Med. 2004;79(6):541–8.
Benjamin RM. Multiple chronic conditions: a public health challenge. Public Health Rep. 2010;125(5):626–7.
Counsell SR, Callahan CM, Clark DO, et al. Geriatric care management for low-income seniors: a randomized controlled trial. JAMA. 2007;298(22):2623–33.
Counsell SR, Callahan CM, Tu W, Stump TE, Arling GW. Cost analysis of the Geriatric Resources for Assessment and Care of Elders care management intervention. J Am Geriatr Soc. 2009;57(8):1420–6.
Reid RJ, Coleman K, Johnson EA, et al. The group health medical home at year two: cost savings, higher patient satisfaction, and less burnout for providers. Health Aff (Millwood). 2010;29(5):835–43.
Gilfillan RJ, Tomcavage J, Rosenthal MB, et al. Value and the medical home: effects of transformed primary care. Am J Manag Care. 2010;16(8):607–14.
Wennberg DE, Marr A, Lang L, O’Malley S, Bennett G. A randomized trial of a telephone care-management strategy. N Engl J Med. 2010;363(13):1245–55.
Boult C, Frank A, Boult L, Pacala J, Snyder C, Leff B. Successful models of comprehensive care for older adults with chronic conditions: evidence for the Institute of Medicine’s “Retooling for an Aging America” report. J Am Geriatr Soc. 2009;57:2328–37.
Peikes D, Chen A, Schore J, Brown R. Effects of care coordination on hospitalization, quality of care, and health care expenditures among Medicare beneficiaries: 15 randomized trials. JAMA. 2009;301(6):603–18.
Berenson R, Devers K, Burton R. Will the Patient-Centered Medical Home Transform the Delivery of Health Care? Timely Analysis of Immediate Health Policy Issues. Washington, DC: Urban Institute; 2011.
Boyd CM, Boult C, Shadmi E, et al. Guided Care for multi-morbid older adults. Gerontologist. 2007;47(5):697–704.
Wolff JL, Rand-Giovannetti E, Palmer S, et al. Caregiving and chronic care: the Guided Care Program for Families and Friends. J Gerontol A Biol Sci Med Sci. 2009;64(7):785–91.
Boult C, Reider L, Frey K, et al. The early effects of “Guided Care” on the quality of health care for multi-morbid older persons: a cluster-randomized controlled trial. J Gerontol A Biol Sci Med Sci. 2008;63(A)(3):321–7.
Pope GC, Kautter J, Ellis RP, et al. Risk adjustment of Medicare capitation payments using the CMS-HCC model. Health Care Financ Rev. 2004;25(4):119–41.
Giddens JF, Tanner E, Frey K, Reider L, Boult C. Expanding the gerontological nursing role in Guided Care. Geriatr Nurs. 2009;30(5):358–64.
Boult C, Giddens JF, Frey K, Reider L, Novak T. Guided Care: A new nurse-physician partnership in chronic care. New York: Springer; 2009.
Ware JE, Kosinski M. Interpreting SF-36 summary health measures: a response. Qual Life Res. 2001;10(5):405–20.
Glasgow RE, Wagner EH, Schaefer J, Mahoney LD, Reid RJ, Greene SM. Development and validation of the Patient Assessment of Chronic Illness Care (PACIC). Med Care. 2005;43(5):436–44.
Safran DG, Kosinski M, Tarlov AR, et al. The Primary Care Assessment Survey: tests of data quality and measurement performance. Med Care. 1998;36(5):728–39.
Angst F, Aeschlimann A, Stucki G. Smallest detectable and minimal clinically important differences of rehabilitation intervention with their implications for required sample sizes using WOMAC and SF-36 quality of life measurement instruments in patients with osteoarthritis of the lower extremities. Arthritis Rheum. 2001;45(4):384–91.
Royston P. Multiple imputation of missing values: update of ICE. Stata Journal. 2005;5(4):527–36.
Thompson SG, Pyke SD, Hardy RJ. The design and analysis of paired cluster randomized trials: an application of meta-analysis techniques. Stat Med. 1997;16(18):2063–79.
Lunn D, Spiegelhalter D, Thomas A, Best N. The BUGS project: Evolution, critique and future directions. Stat Med. 2009;28(25):3049–67.
Boyd CM, Reider L, Frey K, et al. The effects of Guided Care on the perceived quality of health care for multi-morbid older persons: 18-month outcomes from a cluster-randomized controlled trial. J Gen Intern Med. 2010;25(3):235–42.
Marsteller JA, Hsu YJ, Reider L, et al. Physician satisfaction with chronic care processes: a cluster-randomized trial of guided care. Ann Fam Med. 2010;8(4):308–15.
Marteller JA, Hsu YJ, Wen M, et al. Effects of Guided Care on Providers’ Satisfaction with Care: A Three-Year Matched-Pair Cluster-Randomized Trial. Population Health Management 2013 (in press).
Wolff JL, Giovannetti ER, Boyd CM, et al. Effects of Guided Care on family caregivers. Gerontologist. 2010;50(4):459–70.
Boult C, Boult L, Morishita L, Pirie P. Soliciting defined populations to recruit samples of high-risk older adults. J Gerontol A Biol Sci Med Sci. 1998;53(5):M379–84.
Peikes D, Zutshi A, Genevro J, Parchman ML, Meyers D. Early Evaluations of the Medical Home: Building on a Promising Start. Am J Manag Care. 2012;18(2):105–16.
Centers for Medicare & Medicaid Services (CMS). Medicare coordinated care demonstration. 2012. Available at http://www.cms.gov/Medicare/Demonstration-Projects/DemoProjectsEvalRpts/Medicare-Demonstrations-Items/CMS1198864.html. Accessed October 5, 2012.
Brown RS, Peikes D, Peterson G, Schore J, Razafindrakoto CM. Six features of Medicare Coordinated Care Demonstration programs that cut hospital admissions of high-risk patients. Health Aff (Millwood). 2012;31(6):1156–66.
Acknowledgements
We thank: Wade Kramer, MHSA, and Susan Kim, BS, CPA, of Kaiser Permanente; Paula Norman, BS, of Johns Hopkins HealthCare; and Taneka Lee, BS, of the Lipitz Center for the expert technical assistance they provided in the course of their regular employment. We also thank Constantine Frangakis, PhD, and Thomas Louis, PhD, of the Department of Biostatistics at the Johns Hopkins Bloomberg School of Public Health for contributing their assistance with the statistical analysis.
This study was supported by grants from the Agency for Healthcare Research and Quality, the National Institute on Aging, the John A. Hartford Foundation, and the Jacob and Valeria Langeloth Foundation—and by in-kind contributions from Johns Hopkins HealthCare (administrative and information technology support), Johns Hopkins Community Physicians (clinical office space), Kaiser Permanente Mid-Atlantic States (administrative support and clinical office space), MedStar Physician Partners (clinical office space), and the Roger C. Lipitz Center for Integrated Health Care (administrative support).
None of the supporting organizations had any role in: the design and conduct of the study; the collection, management, analysis or interpretation of the data; or the preparation, review, or approval of the manuscript. Drs. Boult and Scharfstein had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Disclaimer
The views expressed in this article are Dr. Boult’s and do not necessarily reflect those of PCORI.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by grants from the Agency for Healthcare Research and Quality, the National Institute on Aging, the John A. Hartford Foundation, and the Jacob and Valeria Langeloth Foundation—and by in-kind contributions from Johns Hopkins HealthCare, Johns Hopkins Community Physicians, Kaiser Permanente Mid-Atlantic States, MedStar Physician Partners, and the Roger C. Lipitz Center for Integrated Health Care.
Clinical Trials.gov ID# NCT0012194
Electronic supplementary matrials
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 14 kb)
Rights and permissions
About this article
Cite this article
Boult, C., Leff, B., Boyd, C.M. et al. A Matched-Pair Cluster-Randomized Trial of Guided Care for High-Risk Older Patients. J GEN INTERN MED 28, 612–621 (2013). https://doi.org/10.1007/s11606-012-2287-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-012-2287-y